Video on What is Periodontal (Gum) Disease?
Video on How do I know If I have Periodontal (Gum) Disease?
Video on Tooth loss due to Periodontal (Gum) Disease
Periodontal Disease FAQ
Periodontal literally means “around the tooth.” Periodontal or gum diseases are serious infections affecting the tissues surrounding the teeth. These tissues include the gums and bone supporting the teeth. Gone unchecked, periodontal disease can result in tooth loss.
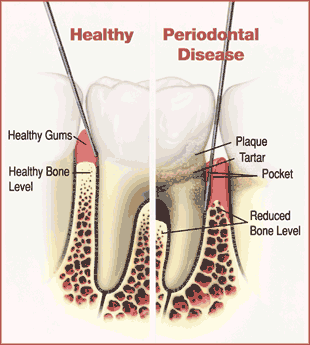
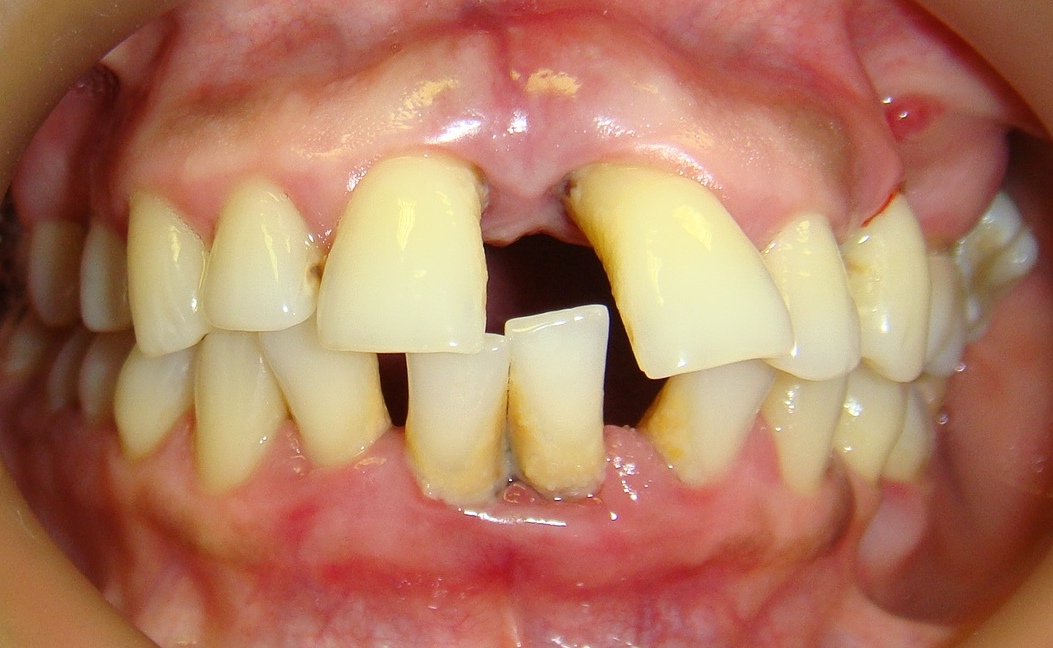
Periodontal disease is usually a slow, painless and progressive disease. Most adults with periodontal disease are unaware they have it.
Periodontal diseases can take a number of years for enough bone loss to occur for the teeth to become loose. However, the severity of the disease can vary from one person to another. Periodontal diseases are classified according to the severity of the disease. The two major stages are gingivitis and periodontitis. Gingivitis is a milder and reversible form of periodontal disease that only affects the gums. Gingivitis may lead to more serious, destructive forms of periodontal disease called periodontitis.
Health
- Coral pink colour
- Gums hug teeth tightly
- No bleeding
Gingivitis
- Bleeding while brushing or during probing
- Inflamed, sensitive gums
- Possible bad breath/taste
Mild Periodontitis
- More pronounced gingival bleeding, swelling
- Gums may begin to pull away from teeth
- Bad breath/taste
- Pockets 3-4 mm deep
Moderate Periodontitis
- Teeth may look longer due to gum recession
- Gum boils or abscesses may develop
- Bad breath, bad taste
- Teeth may begin to drift and show spaces
- Pockets 4-6 mm deep
Advaned Priodontitis
- Teeth may become mobile or loose
- Constant bad breath and bad taste
- Teeth sensitive due to exposed roots
- Pockets > 6mm deep
- Some teeth may be extracted (pulled)
If diagnosed and treated early, however, the teeth can be saved. Treatment becomes more difficult as it progresses but it can be very successfully treated in the earlier stages.
The main cause of gum disease is bacterial plaque, a sticky film that forms on your teeth. Plaque is an often colourless mass of bacteria that sticks to teeth, crowns and bridges, and other tissues in the oral cavity. Plaque is constantly forming on the teeth. Plaque irritates the gums, causing them to become red, tender, and swollen (see picture).
Gum Disease –Bacterial plaque, a sticky film that forms on your teeth.
If not removed daily, plaque becomes the hard material known as tartar or calculus. Calculus cannot be removed by brushing and flossing alone. A dentist, periodontist, or hygienist must remove it manually to stop the disease process.
Gum Disease –Calculus develops below the gums on the tooth roots.
If calculus develops below the gums on the tooth root, it makes plaque removal more difficult, increasing your risk for developing periodontal disease. Toxins (poisons) produced by the bacteria in plaque irritate the gums, causing infection. These toxins also can destroy the tissues supporting the teeth, including the bone. When this happens, gums separate from the teeth, forming “pockets” that fill with even more plaque and more infection. As the diseases progress, these pockets deepen, more gum tissue and bone are destroyed, and the teeth eventually become loose. If periodontal diseases are not treated, the teeth may need to be removed.
The best way to find out if you have periodontal disease is to have your dentist or a periodontist examine your mouth. Many times the common signs, such as bleeding gums and tooth looseness, are not present and the disease goes undiagnosed until the gum disease is very advanced.The clinical diagnosis of periodontitis requires evaluation by a trained examiner and evidence of gingival inflammation, loss of connective tissue surrounding the teeth measured by clinical examination and bone loss detected by radiography.
Use the following questions to see if you may have some of the signs and symptoms indicative of progressive periodontal disease:
- Does your gum bleed when you floss or brush your teeth?
- Are your gums red, tender or swollen?
- Is pus visible when you press on your gums?
- Do your teeth appear to be getting LONGER?
- Is your gum line Uneven when you smile?
- Are the roots of your teeth exposed and sensitive to hot or cold?
- Can you move or wiggle one or more of your teeth with your tongue or fingers?
- Is there S P A C E S between your teeth where there were none before?
- Has there been a change in how you bite?
- Has there been a change in how your partial denture(s) fit(s)?
- Do you have bad breath or a bad taste in your mouth?
The best way to prevent periodontal disease is through effective daily brushing and flossing, as well as regular dental visits that include a periodontal exam and thorough cleaning. If plaque is not removed, it can turn into a hard substance called calculus in less than two days. Calculus, or tartar as this substance is often called, is so hard, it can only be removed during a professional cleaning. Daily cleaning will help keep calculus formation to a minimum, but it won't completely prevent it. A professional cleaning, by a dentist or hygienist, at least twice a year is necessary to remove calculus from places your toothbrush and floss may have missed.
There are many factors other than plaque that contribute to periodontal disease. This means that there is not just one cause of periodontal diseases but rather multiple factors that can affect the health of your gums.
TOBACCO use significantly increases the risk of developing periodontal diseases and can negatively affect treatment.
HORMONAL CHANGES during pregnancy, puberty and menopause can cause the gums to become red, tender and bleed easily.
GENETICS and family history of periodontal diseases indicate a greater likelihood of developing these diseases.
STRESS can make it more difficult for the body to fight off infection, including periodontal diseases.
Some MEDICATIONS such as oral contraceptives, antidepressants and certain heart medicine, can affect oral health.
DESTRUCTIVE HABITS such as improper oral hygiene technique, oral piercing, drug or alcohol abuse can affect periodontal health.
POOR NUTRITION can make it harder for the body to fight off infection.
SYSTEMIC DISEASES that interfere with the body's immune system may worsen the condition of the gums and supporting bone.
Research suggests that the germs that cause gum disease may be transferred in saliva.
Periodontal disease is not cured; in most people, most of the time, it is controlled. Failure to practice good oral hygiene and get the prescribed regular dental cleanings can lead to relapse. Changes in your health may also lead to increased disease susceptibility
Research has shown that periodontal bacteria are associated with cardiovascular disease. Treating your periodontal disease can decrease these bacteria and may decrease the risk of developing cardiovascular disease and other systemic health conditions (such as diabetes and premature low birth weight babies).
Not usually. There may be minor discomfort, which is usually well controlled with local anaesthesia and pain medications. Most patients go back to work and normal activities the day after surgical therapy.
Yes, we can evaluate and treat your periodontal condition without a referral. And if you do not have a general dentist we can refer you to one.
Gingival flap surgery is a type of gum procedure. The gums are separated from the teeth and folded back temporarily. This allows a dentist to reach the root of the tooth and the bone. Gingival flap surgery is used to treat gum disease (periodontitis). It may be recommended for people with advanced periodontitis. Usually, a treatment that doesn't involve surgery is done first. This is called scaling and root planing. If this treatment does not eliminate the gum infection, gingival flap surgery may be used. It also may be done along with another procedure known as osseous (bone) surgery.
There are many types of periodontal diseases. The following is an overview of the most common:
Gingivitis:
As the mildest form of the periodontal diseases, gingivitis causes the gums to become red, swollen, and bleed easily. There is usually no discomfort at this stage.
Chronic Periodontitis:
Chronic periodontitis is a condition resulting in inflammation within the soft tissues surrounding the teeth causing progressive attachment and bone loss (see below pictures). It is diagnosed by bone loss on a dental X-ray, the formation of gum pockets and/or receding gums. It is most common in adults, but can occur at any age.
Aggressive Periodontitis:
This form occurs in patients who are otherwise in good health. Common features include rapid attachment loss and bone destruction. There are two forms of aggressive periodontitis:
LOCALIZED AGGRESSIVE PERIODONTITIS
– Most often occurs near puberty and usually involves attachment loss around first molars and/or front teeth but may involve one or two additional teeth.
GENERALIZED AGGRESSIVE PERIODONTITIS
– Usually, but not always affects people under 30 years of age. It involves attachment loss on at least three permanent teeth in addition to first molars and incisors.
Periodontitis as a Manifestation of Systemic Disease:
As the name indicates, this form is associated with one ofseveral systemic diseases that are related to periodontitis, such as diabetes.
Necrotizing Periodontal Diseases:
These types of periodontal diseases cause ulcers in the gums between the teeth and are most commonly observed in individuals with certain conditions including, but not limited to, HIV infection, malnutrition and immunosuppression. Stress, smoking, and poor oral hygiene sometimes can contribute to this problem.
Click here for Periodontal Diseases Photo Gallery
Video on What is Dental Implant?
Dental Implants FAQ
A dental implant is an artificial tooth root that a dental surgeon places into the jaw to hold a replacement tooth or bridge. Dental implants are an ideal option for people in good general oral health who have lost a tooth or teeth due to periodontal disease, an injury, or some other reason.
While high-tech in nature, dental implants are actually more tooth-saving than traditional bridgework, since implants do not rely on neighboring teeth for support.
Dental implants are so natural-looking and feeling; you may forget you ever lost a tooth. You know that your confidence about your teeth affects how you feel about yourself, both personally and professionally. Perhaps you hide your smile because of spaces from missing teeth.
Maybe your dentures don't feel secure. Perhaps you have difficulty chewing. If you are missing one or more teeth and would like to smile, speak and eat again with comfort and confidence, there is good news! Dental implants are teeth that can look and feel just like your own!
Under proper conditions, such as placement by a periodontist and diligent patient maintenance, implants can last a lifetime. Long-term studies continue to show improving success rates for implants.
Dental implants have become the treatment of choice for replacing non-restorable and missing teeth. Implants offer both functional and esthetic results.
They are the next best thing to your natural teeth in look, feel and function. Implant placement immediately after tooth extraction prevents bone loss in the jaws; maintaining the shape of the face and allowing the return to normal functional use.
Implants have been in use for over 30 years and have a proven success rate for virtually a lifetime of use without any more maintenance than daily brushing and flossing. Dental implants have improved the quality of life for a generation of patients.
Are you missing one or more teeth in a jaw? Are you missing all natural teeth in one or both jaws? Are you having difficulty wearing a regular removable denture because you gag, find the denture is too bulky, feel pain, or generally dislike something movable in your mouth?
Replace a Single Tooth If you are missing a single tooth, one implant and a crown can replace it. A dental implant replaces both the lost natural tooth and its root.
Replace Several Teeth If you are missing several teeth, implant-supported bridges can replace them. Dental implants will replace both your lost natural teeth and some of the roots.
Replace All of Your Teeth If you are missing all of your teeth, an implant-supported full bridge or full denture can replace them. Dental implants will replace both your lost natural teeth and some of the roots.
Success rates vary, depending on where in the jaw the implants are placed but, in general, dental implants have a success rate of up to 97%. With proper care that you would give your regular teeth, your implants can last a lifetime.
Long-term success depends on multiple factors. First, success will depend on the quality and quantity of bone. The greater the quality and quantity of available bone, the greater the chance of long-term success.
Secondly, the experience and ability of the dental surgeon will be a factor. As with any surgical procedure, there is no substitute for the experience and individual talent of the dentist.
Lastly, the quality of the restoration placed on top of the implant will play a big role in long-term success. If the design of the implant crown or overdenture is poorly constructed and the biting forces are not balanced, even the best-placed dental implant will have a compromised survival rate.
The success of your implants will also depend greatly on how well you maintain them. They will need to be professionally cleaned by a hygienist and examined by a dentist every three to four months. Also, brushing and flossing daily is absolutely necessary for long-term implant success.
Improved appearance. Dental implants look and feel like your own teeth. Because implants are designed to fuse with bone, they prevent the bone loss and gum recession that often accompany bridgework and dentures.
Improved speech. With poor-fitting dentures, the teeth can slip and wobble within the mouth, causing you to mumble or slur your words. Dental implants allow you to speak with comfort and confidence. You can also stop worrying about misplaced dentures and messy pastes and glues.
Improved comfort. Because they become part of you, implants eliminate the discomfort of removable dentures or partial dentures.
Easier eating. Sliding dentures can make chewing difficult. Dental implants function like your own teeth, allowing you to eat your favourite foods with confidence and without pain.
Improved self-esteem. Dental implants can give you back your smile, and help you feel better about yourself.
Improved oral health. Dental implants don't require reducing (cutting down) adjacent teeth, as a tooth-supported bridge does. Because nearby teeth are not altered to support the implant, more of your own teeth are left intact, improving your long-term oral health. Individual implants also allow you to floss between the implant and adjacent teeth, improving oral hygiene.
Durability. Implants are very durable and will last many years. They require the same care as real teeth, including brushing, flossing, and regular dental check-ups. With good care, many implants last a lifetime.
Convenience. Removable dentures are just that; removable. Dental implants eliminate the embarrassing inconvenience of removing your dentures, as well as the need for messy adhesives to keep your dentures in place.
Reliable. The success rate of dental implants is highly predictable. They are considered an excellent option for tooth replacement.
Great value. Dental implants are also a great value for your investment. You will be getting a product that you will be using 24 hours a day, 7 days a week, 52 weeks of the year, probably for many, many years of your life.
Individualized Treatment Plan. The first step in the process is the development of an individualized treatment plan. The plan addresses your specific needs and is prepared by a dental team of professionals who are specially trained and experienced in oral surgery and restorative dentistry. This team approach provides coordinated care based on the implant option that is best for you.
Implant Site Preparation. Since a key to implant success is the quality and quantity of the bone where the implant is to be placed, sometimes bone grafting is necessary in order to prepare the bone for an implant.
Extraction Site Grafting: Bone grafting in extraction sites helps preserve jaw height and create sufficient bone foundation for future implant placement(s).
Ridge Augmentation: Deformities in the upper or lower jaw can leave you with inadequate bone in which to place dental implants. To correct the problem, the gum is lifted away from the ridge to expose the bony defect. The defect is then filled with bone or bone substitute to build up the ridge. Ridge modification has been shown to greatly improve appearance and increase your chances for successful implants that can last for years to come.
Sinus Augmentation: The upper molar area is usually one of the most difficult areas to place dental implants because of insufficient bone quality and quantity and proximity to the sinus. Sinus augmentation can help develop more bone in this area by raising the floor of the sinus and adding bone grafting material in the area of proposed implant placement.
Implant Placement. The tooth root implant, which is a small post made of titanium, is placed into the jaw bone in the position of the missing tooth or teeth. As the bone heals, it grows around the titanium post, anchoring it securely. The healing process usually takes from 3-6 months.
Permanent implant restoration Once the implant has bonded to the bone, a small connector post – called an abutment – is attached to the implant to securely hold the new tooth. To make your new tooth or teeth, your dentist takes impressions of your teeth and creates a model of your bite (which captures all of your teeth, their type, and arrangement). Your new tooth or teeth are based on this model. A dental crown is then attached to the abutment. The implant is secured within the jawbone, the replacement tooth looks, feels, and functions just like your own natural tooth.
As with other dental procedures, an effective local aesthetic is used during implant surgery to minimize any discomfort during the placement of the implants. Postoperative care includes prescription pain medication. However, many patients require only over-the-counter Neurofen. You can usually go to work the next day after implant surgery.
As with many surgical procedures, dental implant fees will vary. Frequently, a more experienced implant dentist will charge higher fees. Each individual implant dentist will be able to quote you his fees. It is important to remember that there are two different implant fees: Surgical fees (placement of implant by the dental surgeon) Restorative fees (placement of abutment post and dental crown by the restorative dentist)